
About Stimpod NMS460
The Stimpod’s patented waveform is delivered transcutaneously and affects the cellular metabolic activity of a neuropathic nerve. The induced electromagnetic field propagates as short bursts and travels along the axons to the spinal dorsal horn, restoring intra-neural communication pathways and natural nerve functionality.
Nerve locating technology allows you to find the affected nerve through the skin. Accurate placement of the treatment probe is confirmed by muscle twitches for motor nerves and patient feedback for sensory nerves.
Quick Start Guide
Stimpod NMS460 Features
Long term relief from chronic pain
Restores natural nerve functionality
Fast onset of action
No side-effects
Specialist training for DCs, MDs and PTs
Portable and easy to use
Backed by multiple clinical trials
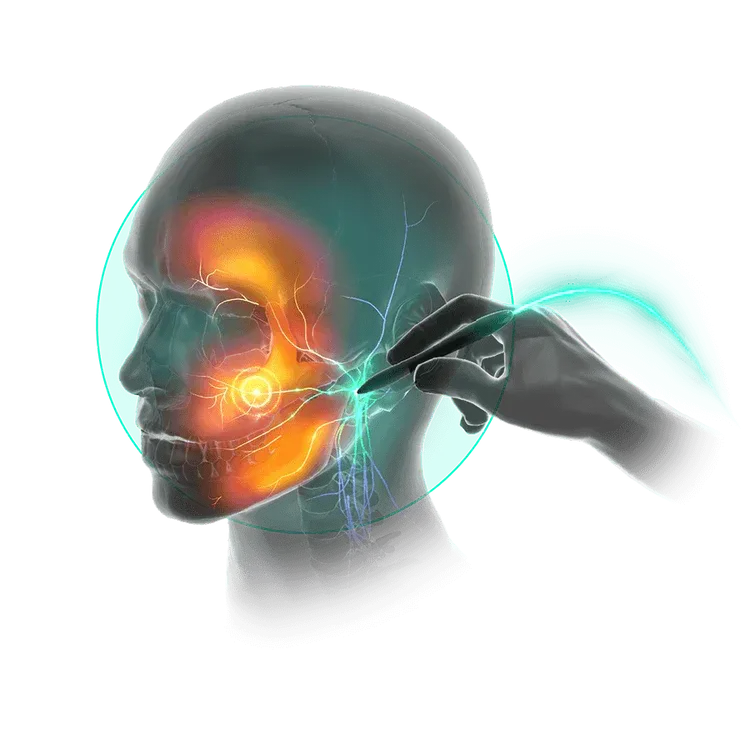
World's First Non-Invasive Pulsed Radio Frequency Treatment System
The Stimpod is indicated for:
The symptomatic relief and management of chronic intractable pain
An adjunctive treatment in the management of post-surgical pain
An adjunctive treatment for post-traumatic, acute pain problems
An adjunctive treatment for pain control due to rehabilitation
